
AI CERTS
3 hours ago
Healthcare Predictive Analytics: Forecasting Heart Failure via AI
However, gaps remain around deployment, regulation, and workforce readiness. This article examines cutting-edge evidence, emerging products, and practical considerations shaping this rapidly evolving field. Industry professionals will gain actionable insights and resources for strategic planning. Meanwhile, clear next steps will be highlighted for successful implementation. Ultimately, the goal is improved outcomes and sustainable health-system value. Therefore, careful translation of data into practice is essential.
Global Burden Drives Demand
Heart failure now affects about 6.7 million adults in the United States alone. Furthermore, the condition accounts for roughly nine percent of cardiovascular deaths each year. Hospital admissions consume billions in annual costs, straining payers and providers alike. In contrast, early identification can reduce admissions and slow disease progression. Healthcare Predictive Analytics promises scalable screening that catches ventricular dysfunction before congestion escalates. Consequently, policymakers and investors are prioritizing tools that triage risk in community settings. These drivers create fertile ground for algorithmic innovation.
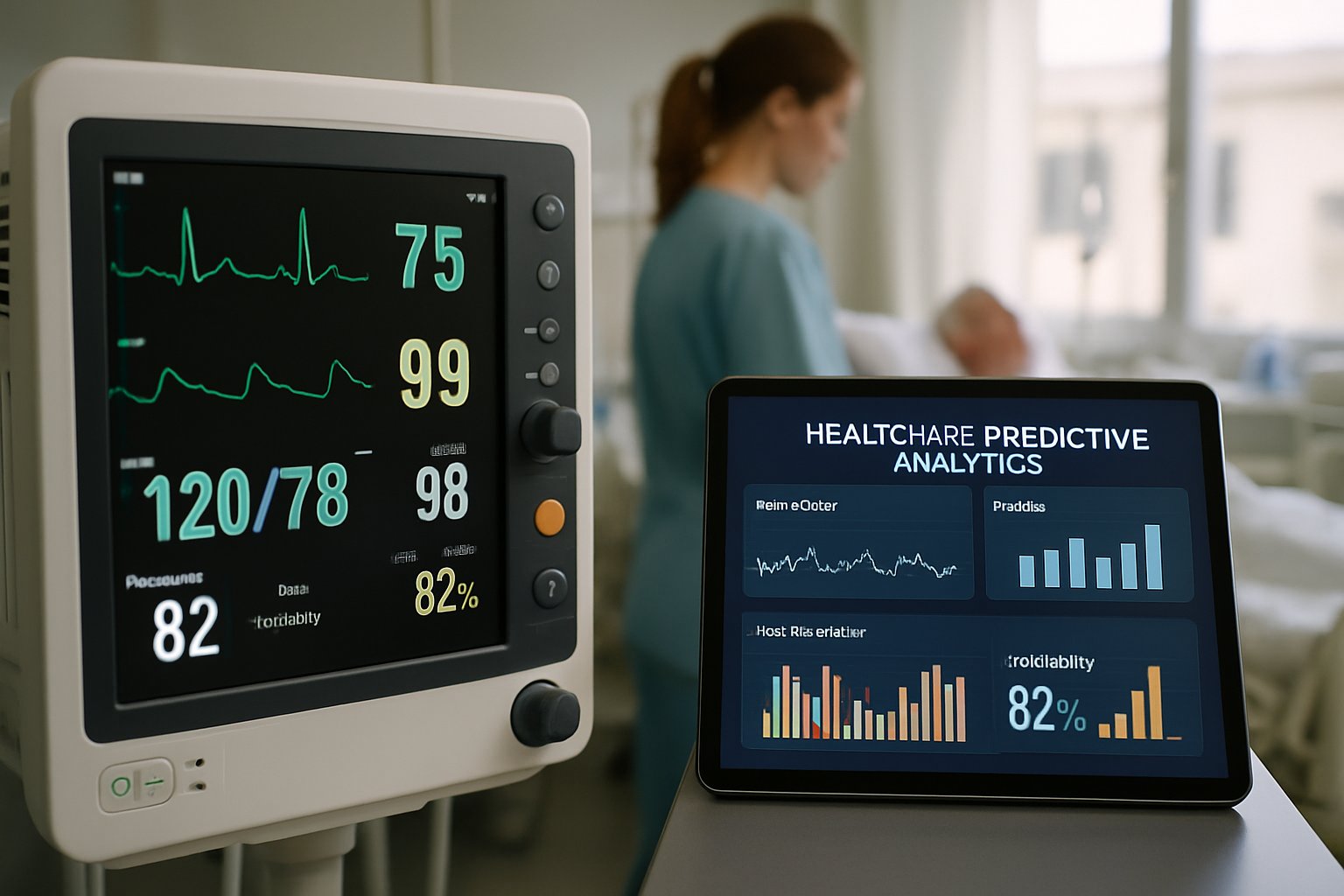
Global epidemiology underscores an urgent need for accurate, low-cost risk stratification. Accordingly, researchers have focused on electrocardiograms as an accessible data source. The following section explores how AI-enhanced ECGs are maturing toward clinical deployment.
AI-ECG Models Mature
Retrospective cohorts from Yale, UK Biobank, and ELSA-Brasil total more than 248,000 participants. Moreover, a noise-adapted single-lead model delivered Harrell C statistics between 0.72 and 0.83. Positive screens correlated with three- to seven-fold higher risk of first Heart failure hospitalization. Importantly, Healthcare Predictive Analytics improved discrimination when combined with established PCP-HF and PREVENT scores. Nevertheless, external validation remained strong across diverse geographies and device vendors. Clinicians appreciate that a single quick ECG could guide further natriuretic peptide testing or imaging. Accurate prognosis helps allocate specialist visits to those most likely to deteriorate.
Key performance numbers illustrate current readiness:
- Harrell C up to 0.83 across three cohorts.
- Hazard ratios ranged 3.9–23.5 for incident HF.
- Incremental C gain over PCP-HF reached 0.05 in test sets.
- Screening time per ECG remained under one second.
Consequently, many hospitals now pilot AI-ECG dashboards within electronic records. Yet, prospective outcome trials remain scarce. These multicenter results confirm technical validity and spark confidence among cardiologists. However, wearable data streams promise even richer longitudinal insight, as the next section reveals.
Wearables Enable Hemodynamic Insights
The MIT-Harvard CHAIS model analyzed single-lead patch recordings to infer left atrial pressure. Internal AUC reached 0.80, while external cohorts achieved 0.76. Additionally, a prospective subset near catheterization posted an impressive 0.875 AUC. Therefore, continuous ambulatory monitoring could alert clinicians before decompensation episodes. Healthcare Predictive Analytics platforms already integrate patch data with medication adherence alerts.
Moreover, algorithmic scores can trigger telehealth visits or diuretic titration protocols. Still, false positives risk unnecessary escalation if clinical pathways are vague. Industry observers believe reimbursement for remote hemodynamic monitoring will decide commercial viability.
Wearable sensors expand temporal coverage and personalize risk curves. Subsequently, imaging data provide complementary structural context, discussed below.
Multimodal Imaging Strengthens Prognosis
Deep learning has transformed chest radiographs and echocardiograms into predictive biomarkers. For example, convolutional survival networks reach C-indices near 0.80 for mortality and Heart failure events. Moreover, combining ECG, CXR, and EHR variables yields higher net reclassification improvement versus single modality alone. Healthcare Predictive Analytics vendors now offer dashboards that merge imaging and waveform outputs. In contrast, many radiology departments still lack integrated reporting pipelines. Strategic Healthcare Predictive Analytics roadmaps now highlight imaging as a critical pillar. Nevertheless, cloud deployment models reduce on-premise computing barriers.
Clinical teams value several advantages:
- Rapid ED triage within minutes of X-ray capture.
- Objective severity scores support early ICU transfers.
- Automated longitudinal graphs track ventricular remodeling trends.
Yet, explainability and liability questions persist. Multimodal models sharpen prognosis and guide resource allocation. However, benefits materialize only when ethical and operational pitfalls are addressed next.
Risks And Deployment Challenges
Algorithmic bias remains a foremost concern among regulators and ethicists. Indeed, retrospective training sets often underrepresent minority populations and women. Consequently, miscalibrated scores could widen disparities in Heart failure management. Furthermore, unclear follow-up pathways can foster alarm fatigue and unnecessary repeat imaging. Prospective impact studies must evaluate cost, anxiety, and downstream utilization, not just discrimination.
Healthcare Predictive Analytics initiatives should embed fairness audits, calibration checks, and stakeholder governance early. Robust Healthcare Predictive Analytics governance frameworks mitigate many deployment risks. Meanwhile, medico-legal frameworks lag behind rapid algorithm iteration cycles. Nevertheless, FDA draft guidance on change control and real-time learning is progressing.
Addressing bias, workflow, and oversight is vital for safe scale-up. The next section examines workforce readiness and education strategies.
Upskilling The Clinical Workforce
Clinicians require fluency in model outputs, limitations, and appropriate escalation protocols. Moreover, multidisciplinary teams must coordinate cardiology, informatics, and nursing perspectives. Healthcare Predictive Analytics training programs are emerging in fellowship curricula and CME courses. Professionals can upskill through the AI Healthcare Specialist™ certification.
Additionally, vendor sandboxes allow safe experimentation with de-identified datasets before bedside rollout. Clear dashboards translate model prognosis into color-coded action thresholds. Hospitals benefit when champions translate technical jargon into actionable clinical steps. Consequently, adoption curves steepen and project ROI improves.
Targeted education ensures algorithms augment, rather than confuse, busy clinicians. Finally, strategic roadmaps must tie all elements together, as the conclusion outlines.
Conclusion And Next Steps
Deep learning innovations are redefining cardiovascular risk stratification and Heart failure care pathways. Healthcare Predictive Analytics already demonstrates strong technical performance across ECGs, wearables, and imaging modalities. However, clinical impact hinges on prospective evidence, equitable design, and clear operational protocols. Stakeholders should prioritize unbiased datasets, robust governance, and continuous education. Moreover, collaboration with regulators and payers will accelerate sustainable reimbursement models.
Therefore, now is the time to pilot scalable solutions and measure real-world outcomes. Readers seeking deeper competence should consider the linked certification and follow upcoming trial results. Consequently, informed leaders can turn algorithmic promise into measurable patient benefit.



